It was an operation that earned him acclaim, but the world’s first heart transplant also provoked hate mail and outspoken criticism of South African surgeon Christiaan Barnard, 50 years ago.
Critical letters
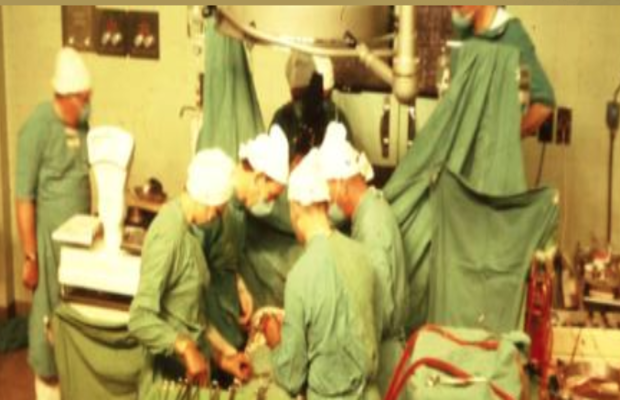
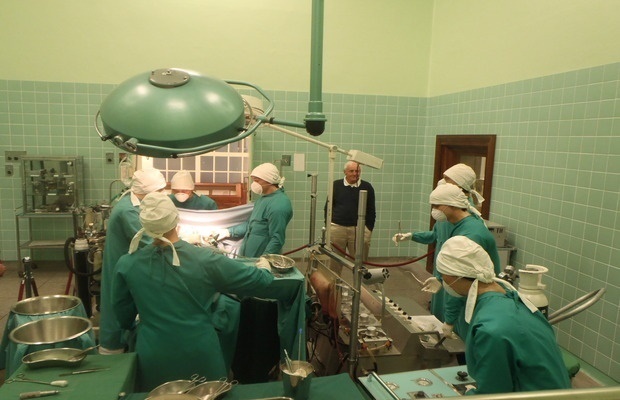
“We did not realise that it would take the public by storm and create such an outcry,” says Dene Friedmann, a specialist nurse on the cardiovascular team, standing in the same Cape Town operating theatre where the medical feat took place.
Its watery-green tiled walls, visited by schools and the public, stir many memories for her of the historic procedure – and its aftermath.
“There were people who wrote quite critical letters to Professor Barnard, horrible letters calling him ‘the butcher’,” says Friedmann, now in her seventies.
It rained insults
“I have heard of human vultures, but it is the first time I have saw one with a name on it,” said one letter dated just one month after the operation and sent from Illinois in the United States.
“You had the audacity to assume the authority of God by pretending to become the giver of life,” said another from Hong Kong.
The French magazine Paris Match summed up the ethical debate in a headline: “The battle of the heart. Do surgeons have the right?”
But the scientific community welcomed the technical advance – the United States had also been seeking the accolade – and ordinary citizens sent congratulations.
A political dimension
At the time the heart was not considered a mere organ – it was more a symbol of deeper meaning, for some, the bringer and taker of life itself.
Unlike today, there was no common legal definition of brain death and the surgical team did not want to be accused of removing a beating heart to give it to another human.
There was also a political dimension, with South Africa’s apartheid government delighted to have some good news.
“They used Professor Barnard as the ambassador for the country,” recalls Friedmann.
‘Empty chest’
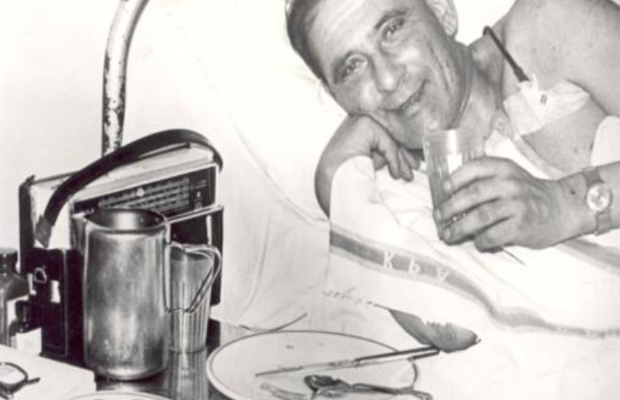
It was on the first floor of Groote Schuur Hospital on December 3, 1967 that Louis Washkansky received the donor heart of Denise Darvall, the 25-year-old victim of a road accident.
Darvall’s father had agreed to the procedure. In the operating theatre Friedmann leaned in to assess Washkansky on the table.
“I looked into this empty chest with no heart in it, a man lying there without a heart in his body and just a lung heart machine keeping him alive. It was very scary,” she says.
In the room next door, Barnard ordered that Darvall’s ventilator be turned off. After about 12 minutes her heart stopped beating and it was quickly moved to the theatre where 53-year-old Washkansky awaited it.
“There were still a lot of medical ethics issues. It was the first time time that a heart transplant was being done… and he did not want anybody to be able to say we took out a beating heart from a patient,” Friedmann says of Barnard, who died in 2001.
“There was a feeling of nervousness: is this heart going to beat and take over the circulation? When it started, it was so exciting, so wonderful.”
The rhythm of life
Barnard, then 45, said of the operation: “The heart lay paralysed, without any sign of life. We waited – it seemed like hours – until it slowly began to relax. Then it came like a bolt of light.
“There was a sudden contraction of the atria, followed quickly by the ventricles in obedient response. Little by little it began to roll with the lovely rhythm of life.”
Coming as it did during the apartheid years race became a consideration when selecting a donor, but only to avoid allegations of prejudice.
The pioneering operation could in fact have been performed weeks earlier, when a coloured man’s heart became available.
“Professor Barnard had decided that the first donor had to be a white person, because of apartheid. We did not want anyone to say ‘You are taking out a black person’s heart to put it in a white patient’,” says Friedmann.
Collapsed immune system
She also squashed the rumour that persists about a black South African, Hamilton Naki, participating in the first transplant but that he was deprived by the apartheid government of any recognition.
“He was very talented, but he never operated on patients,” says Friedmann, who worked with Naki on many laboratory tests on dogs.
Just 18 days after the world first of the Washkansky operation, the patient died. The autopsy revealed that his lungs gave out, but not the heart, because his immune system had collapsed, resulting in pneumonia.
Today, a heart transplant – while still a high-risk procedure – no longer makes headlines.
Around 3 500 transplants are carried out each year, of which about 2 000 are in the United States.
About 88% of patients survive the first year after surgery, 75% survive for five years, and 56% 10 years after the operation, according to the US National Heart, Lung, and Blood Institute (NHLBI).
Image credit: Wikimedia Commons