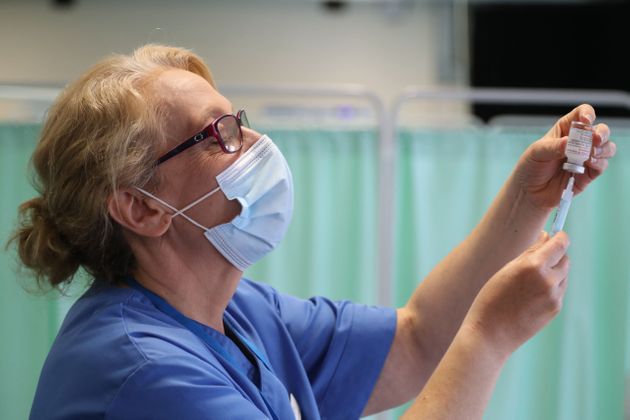
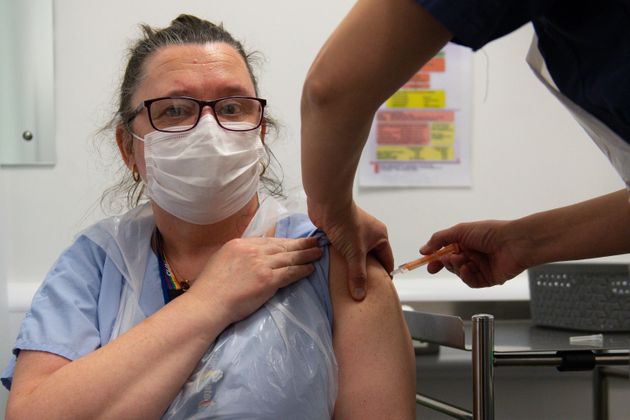
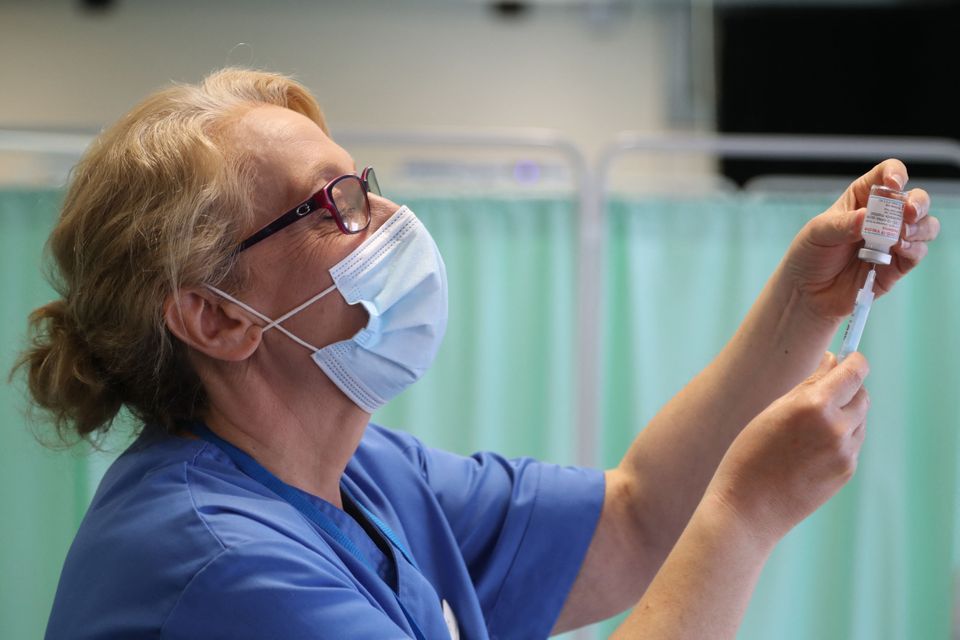
It is hard to explain what it is really like to work as a nurse inside a hospital. The experience is almost impossible to understand unless you have lived it. There is no real-world equivalent to a bad shift in nursing.
Most people do not understand how working three days a week can drain a person so deeply that they spend their days off unable to function. Or why night shift nurses sleep through almost their entire stretch of days off. Or why we cannot always be fully present for our families.
Advertisement
The answer is exhaustion — physical, mental and moral.
When I graduated, I knew nursing would be difficult, but I did not understand what difficult truly meant. My first medical-surgical job showed me immediately. Our ratio was eight patients to one nurse. The charge nurse, the person meant to be the extra support, also carried a full patient load.
Normal was med passes that took hours, often starting one round of medications before finishing the last. Normal meant having to push charting to the end of the shift, and hoping your documentation made sense when you were already 15 hours into a 12-hour shift. Breaks were rare. Getting to go to the bathroom was luck. There was no time to think, much less feel.
Early in my career, one of the most capable nurses I knew accidentally gave the wrong medication to a patient because she was drowning in the workload. Instead of asking what changes could prevent something like that from happening again, our manager asked me what I thought. I was a brand new nurse. I told the truth: The system set her up to fail. She has eight patients. No one can do this safely.
Advertisement
He looked at me and said, “If that is your opinion, you are never going to make it in nursing.”
I carried that moment with me for years. It was the first time I understood that in hospital culture, leadership said the right things about honesty and safety, but the reality did not match the words. Speaking up about real problems was treated as an inconvenience. Vulnerability was something you were expected to swallow. What mattered was endurance.
Eventually, I moved into paediatrics. The ratio was better, but it wasn’t any less intense. Children can look fine one moment and be critically unstable the next. Parents needed reassurance, explanations and someone to translate what was happening. It was a different kind of emotional work.
When the pressure mounted, communication was always the first thing to break. Once, a child went to surgery and never returned to the room. No one told the parents or the unit that the child had been transferred to the ICU. They waited quietly, expecting their child to come back until I told them their child was in intensive care and that we needed to go immediately. Under normal circumstances, someone would have updated them. It was another cut.
Advertisement
I asked leadership whether anyone was tracking these lapses. In every setting I had worked before, investigating what went wrong was standard practice. Leadership told me someone, somewhere, was handling it. It never felt like an answer.
So I moved into leadership as a house supervisor, where I could see the hospital from the top down. I believed that if I could understand the system at a higher level, maybe I could help fix what was breaking.
Instead, I learned how powerless we really were.
As house supervisor, I existed between two worlds. Floor nurses often blamed me for every gap in staffing. Upper leadership expected me to justify every instinct I had. If I believed a unit needed more help, even as I could feel the tension rising on the floor, I had to wake up a director in the middle of the night and explain why. Most of the time, the answer was no.
Advertisement
But the hardest part was not staffing. It was enforcing policies I no longer believed in.
People imagine a nurse quits after one traumatic night or a tragic patient death. That is not how it happens. Most of us enter nursing because we want to help people, because we believe it is our calling, because we think we can make a difference. What breaks you is not one catastrophe. It is the accumulation of moments when you knew what should have been done and were not allowed to do it.
There were nights when I had to walk into a room with security behind me and tell a family member they had to leave. Not because the situation was unsafe. Not because they were disruptive. But because the rulebook said they could not stay.
One night stands out more than any other. A parent begged me to let both of their children stay. One child had been admitted. The other could not be left alone. They pleaded for them to remain together. I called leadership and asked for an exception. I was told there were no exceptions.
Advertisement
I was placed in the position of having to enforce a rule that would separate a family in the middle of the night, with one child remaining in the hospital and the other sent home. That was the moment I knew I was not practicing nursing anymore. I was enforcing rules that made no human sense. Rules that hurt families. Rules that I could not find a way to defend.
Burnout did not hit me all at once. It settled into my body and refused to leave. I began experiencing chest tightness and hyperventilation on the drive to work. I had my heart checked, but I knew it was not cardiac. Panic attacks mimic heart failure. I had seen enough of both to know the difference.
I thought stepping into leadership would give me the tools to fix what was breaking. It did not. The panic worsened. That was when I realised I did not need a new unit or a new specialty. I needed a new life. Something quieter. Something more human.
Advertisement
So I left.

Photo Courtesy Of Melissa Main
Public health felt like the one corner of nursing where the stakes were not life or death every single minute. I moved to a rural county where many families lived off-grid, and I became the only public health nurse for the region. I imagined helping with water access, housing instability, food shortages and clothing needs. My family started our own life in Michigan in a camper, filling five-gallon jugs by hand and navigating limited heat and water, so I understood the community.
But even in public health, the work was limited by funding and politics. Instead of addressing big problems, I found myself focused on vaccines, birth control and disease contact tracing. All important, but much smaller scale than the work the community needed. Then the funding cuts began. Programs froze. Jobs were eliminated. Leadership reminded us every few months that no one’s job was safe, not even theirs. Instead of building long-term public health, we were waiting for the next round of layoffs.
Advertisement
Then the shutdown happened, and the writing was on the wall. How do you serve a community when the structure meant to support it is being dismantled faster than you can help? I realised I could not keep practicing nursing inside systems that were dissolving beneath me.
We say nurses “leave the profession,” but you never really do. I did not stop being a nurse, but I stepped to the side of nursing.
Out here in the woods, I began to feel like myself again. I wake with the sun. I tend to the animals who depend on me. Building a homestead was not only survival. It became a new way to serve. When I gather eggs or bottle-feed calves, I am reminded that even now, in small ways like giving free eggs to neighbours, I am building the kind of community I always wanted. A community where people support one another directly instead of relying on systems that continue to fail them.
Advertisement

Photo Courtesy Of Melissa Main
But this story is not about me. It is about the nurses still showing up every day to a system full of cracks they did not create but are expected to hold together. They deserve a health care system that cares for them with the same intensity they give to everyone else.
Instead, nurses across the nation are watching their profession be reclassified so that the education required for it is no longer considered a professional degree. The wording alone is in poor taste, and it lands like salt in a wound that nurses have never been given the time or space to heal. For many of us, it is one more reminder that the system does not value the work we do.
Advertisement
I have built a peaceful life, one that lets me breathe. But nurses should not have to leave the bedside to save themselves. Nurses do not need more resilience. What they need is support, respect and a health care system that gives them a reason to stay.