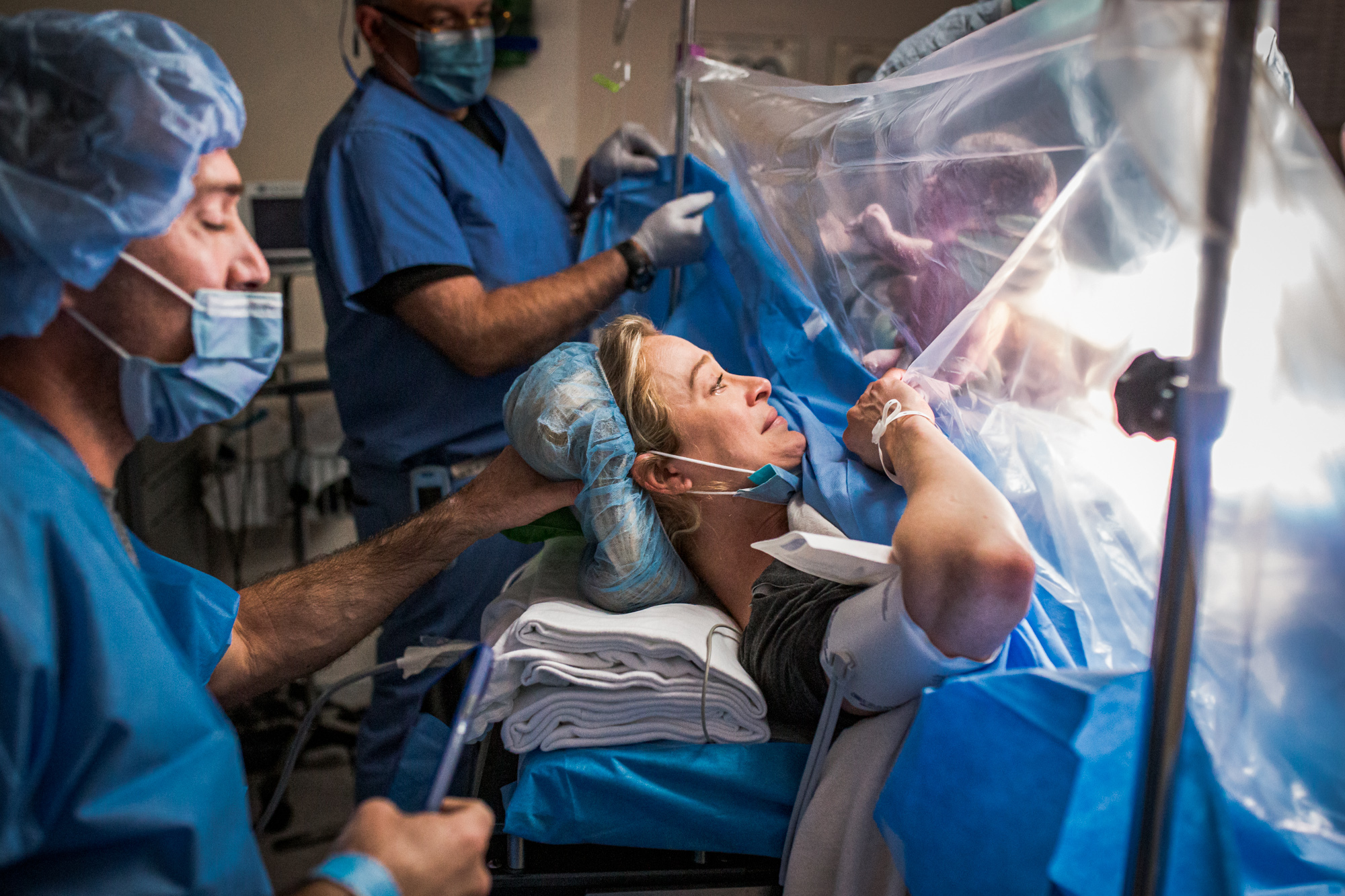
On the first day of school, teachers often send a message to parents in the form of a letter or an email. They include things that students will need for the class, highlights of the year ahead, and how to contact them.
Email, mobile phones and a growing number of school communication apps means that it’s easier than ever before for parents to get in touch with teachers.
Questions, requests, complaints – veteran teachers have heard it all. But, sometimes, parents ask for things that are well outside of the realm of any teacher’s job description.
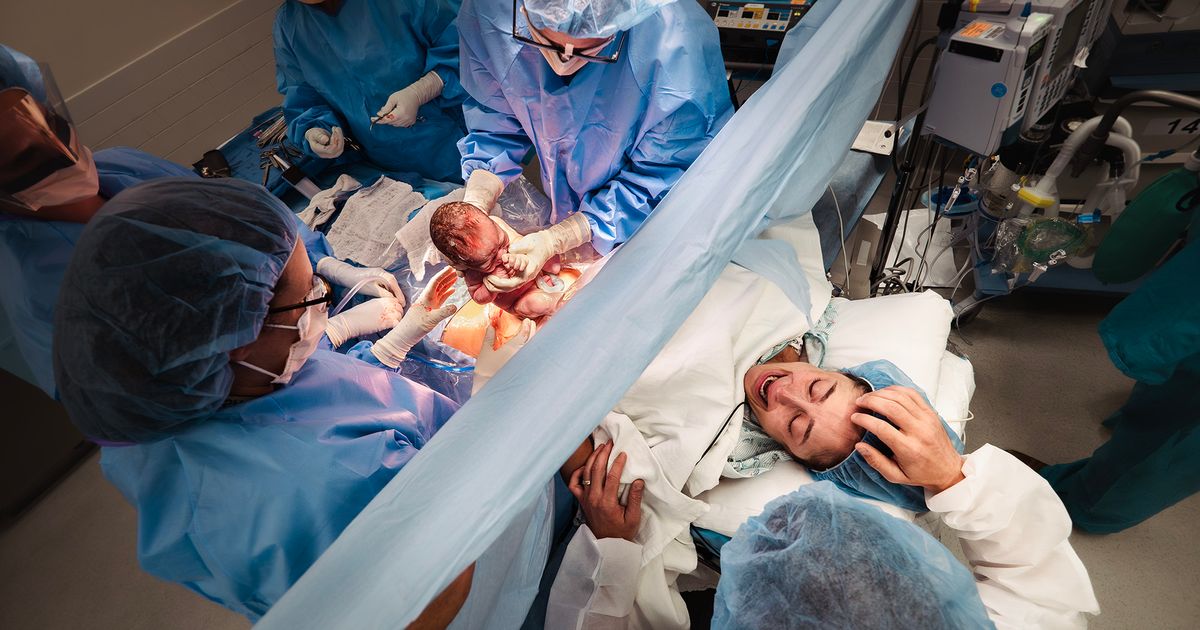
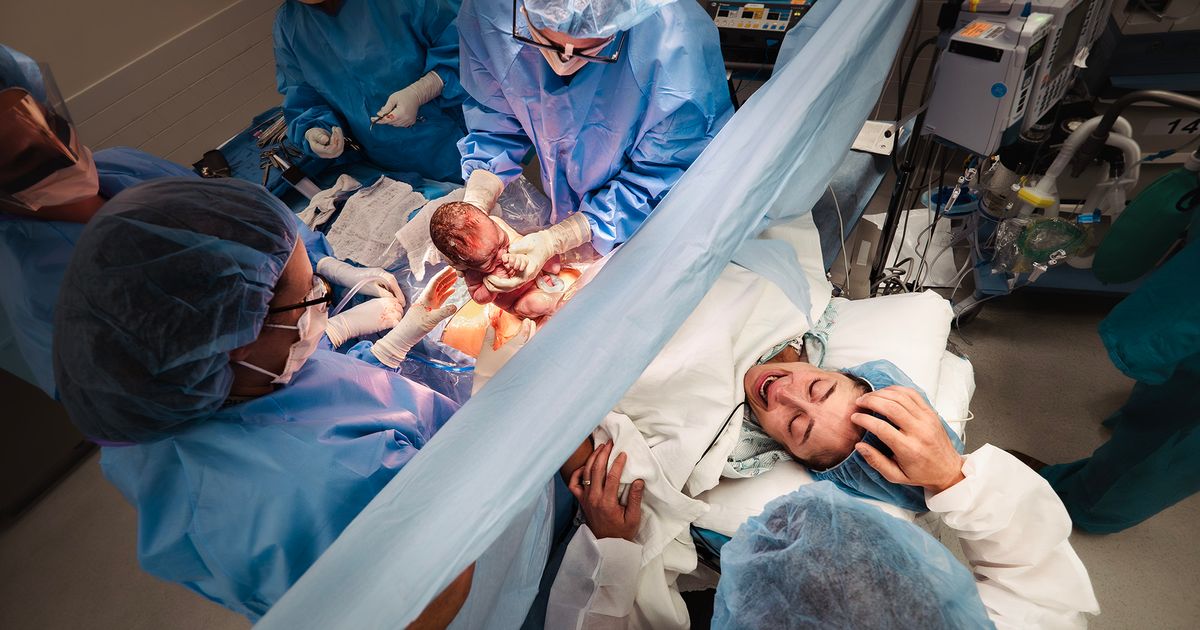
Jane Morris, a Maryland educator whose online presence is known as Teacher Misery, created a video a few years ago featuring fifth-grade teacher Deandre Rashard as he reacted to a series of actual requests from parents that are too wild and bizarre for anyone to have fabricated.
They included: “My son swallowed a watch battery at home. Please use this fork and clothes pin to inspect his poop until we find the battery.”
Others asked teachers to clean their child’s nose on picture day, track a student’s menstrual period and “mood changes,” and squeeze a student’s head during test-taking to relieve anxiety.
Perhaps most galling were requests in which the parents assumed they had greater pedagogical knowledge than the teacher, like the parent who requested that their son be given credit for an essay in spite of not turning one in because he “wrote it in his head.”
HuffPost asked teachers in our HuffPost Parents Facebook community to share their most memorable requests and complaints from parents. Here are some of their responses:
“One time I had a parent email me and ask if their student could take an upcoming math test on a different day because they had a golf tee time scheduled during the test. The student wasn’t on a golf team, nor were they a junior professional, they just wanted an afternoon of golf!”
— S., middle school math teacher in California
“I had a note from a parent to ‘excuse her son from activities if the weather was over 63°’ because he didn’t like to sweat. I also had a note from a dad who said ‘M is on her period today. She said she cannot do any running or physical activity. I told her it would be good for her. She screamed at me. Good luck.’”
— Alaina, middle school P.E. teacher in California
“Parent calls to inform me that their child swallowed a ring the night before and the doctor informed them that it was too far down to be of concern, however they needed to check the child’s bowel movements for the ring to make sure it passed through their system. I was asked to collect any poop and look at it to see if I could find the ring.
We were asked to wash, dry, and change socks of a student each time we came into the classroom because the ‘sand irritates’ her feet. They choose a school whose playground is 100% sand and we go outside four times a day.”
— Christine, pre-K through third grade teacher in New York
“I had a parent some years back who wanted me to chart every day if their child pooped. They also wanted me to keep track of what the child ate at lunch. Child was having digestive issues. Instead, we suggested that they ask child when they got home and they send lunch every day with directions to return all uneaten food for parents to see.”
“I once had a parent complain to admin that they liked last year’s teacher much better. I looped with them from 1st to 2nd ”
— Melissa Gartside, Connecticut
“Mom wanted to put on the IEP that me (special ed teacher) and the occupational therapist would go to their house and teach their very capable autistic 4th grader how to shower more independently. ”
— Jen Monahan, K-5 special education teacher
“I once had a parent accuse me of eating their kids lunch and claimed they had an audio recording of me doing it. ”
“I had a father request a meeting with me and the principal. The father wanted his son moved to a seat by another pencil sharpener. (I had two very expensive electric pencil sharpeners in two different places in my room — that I bought with my own money). The son claimed that sharpener closer to his seat ate up his pencils. Truth was he wanted to move closer to his buddy who was right by the other sharpener. I was told to move the student where he wanted.”
“Mom complained to my principal because she didn’t like my fun Friday bubblegum font. I had to change it ”
“Since my child sees a speech pathologist for the half hour after lunch, I’d appreciate it if you didn’t ‘teach anything new’ until he returns to the classroom.”
“I teach kindergarten. I had a mom email me to tell me that she didn’t think her son was drinking enough water throughout the day. She asked me to check the toilet after he used the bathroom each time so I could monitor the color of his urine and report back to her.”
— Maressa Brooks Rousslange
“Mom sent in a bar of soap. The student, who was a large male, said I was to wash his mouth with soap if he used bad language.”
— Pamela Robison Duren, fourth-grade teacher in California
“When I taught middle school, parent wanted me to make a 60% a ‘B’ because maybe that’s the best the student could do. I had to break it to her that I didn’t create the grading scale.”
“Can you stand over him every class and make sure he does his assignment?”
— Maribeth Jones, high school French teacher
“I had a dad give his first grade son a laxative before school. He sent him with pull ups and wipes and asked if I could help clean him up after.”
“I had a mother ask me to keep an eye on how much her son played a game on his phone and report back to her regularly because he was racking up crazy charges on in-app purchases — north of $400. As long as his phone wasn’t out during my class, it’s not my place to monitor an 18 year old’s device usage.”
— Jason D. Moore, high school graphic design teacher in New York
Responses have been lightly edited for length and clarity.