As we pulled into the parking lot, space No. 8, I tried to tell myself that this was all one big misunderstanding.
“Hopefully this doesn’t take too long,” I told my husband and our chocolate Labrador, Bill. In September 2022, we were still parking outside in an allotted spot and calling the veterinarian’s office to let them know we had arrived before entering the building.
Advertisement
Bill bounced around as the technician took down his vitals. “There is no way my dog, the one sitting here begging for treats and attention, has cancer,” I thought to myself, almost numb to the questions we were being asked, like if Bill still ate.
“Yes, of course he still eats,” I wanted to scream. “He also still plays and pulls on the leash during walks and barks at anyone he sees on the sidewalk.” But the words were trapped in my throat, tucked beneath my N95 mask.
We found ourselves in the veterinary oncology office after our 6-year-old dog developed a cough. I had taken Bill to his primary veterinarian, fully expecting an antibiotic and a $500 bill. Instead, she told me his lymph nodes were slightly enlarged and she was going to aspirate them “out of an abundance of caution.”
“Sometimes it’s cancer,” she said casually, “But Bill is young and healthy.” Those words would haunt me.
Advertisement
When the oncologist came into the room, she confirmed what I was wishing against: Bill had B-cell lymphoma, a cancer that’s treatable, but incurable. Left untreated, he had weeks to live. With treatment, we could hopefully get a year or more.
Just three months prior, my husband and I experienced our fourth consecutive pregnancy loss within an 18-month period, coupled with the devastating news we would not be able to have children of our own. A lymphoma diagnosis for one of our dogs felt like a cruel blow from the universe.
During my fourth pregnancy, I spent months in bed fighting for my life and the one inside of me. Bill would curl his body up against my shoulder so I could rest my head against his back. I’d crawl to the bathroom, too weak to walk, and he would follow, resting his head on my feet.
The upside, the doctor told us, is that chemotherapy doesn’t manifest in dogs the same way that it does humans. Because it’s used to preserve quality of life – not be curative – Bill would never know he was sick, he wouldn’t lose his hair, and any mild side effects, like an upset stomach, could be well managed.
“Some lymphoma patients have lived a long time,” she said.
“That will be Bill. He will be the outlier,” I thought to myself.
And so began the fight for Bill’s life – one that I will be forever grateful to have had the opportunity to endure. Choosing to fight Bill’s lymphoma was a privilege, as it comes with a price tag that is simply not feasible for many families, and we are endlessly grateful we had the ability to make that choice. Surely, a dog who had walked through hell alongside us ― including licking tears off my face as I miscarried my third pregnancy on the bathroom floor at home ― deserved to have his paw held through his own battle. For us, there was no Plan B.
Advertisement
Bill got his first treatment on his seventh birthday. Chemotherapy treatment was new to both my husband and myself. I feel most prepared ― and capable ― when I’m armed with knowledge, so I showed up to Bill’s chemotherapy each week ― always parking in spot No. 8 ― with a list of questions. Our family developed a routine of weekly chemo appointments, and fostered a relationship with his care team that resembled old friends, not medical staff.
After five months, Bill completed his chemotherapy plan, donning a graduation cap, and we cheered in the parking lot as he raced to greet us. We spent two cancer-free months together before the cancer returned. Determined to enjoy more time together as a family, Bill began another chemotherapy protocol that kept us in a state of bliss for more than six months. In some ways, Bill’s lymphoma diagnosis put a dog’s already-too-short lifespan into hyper-focus and left us wondering: How can we make every day his best day?

Photo Courtesy of Kait Hanson
Everything about the 13 months we gained thanks to treatment was an intentional effort to savour joy in both big and small moments. My husband and I began taking both of our dogs with us wherever we went, like car rides to get “pup cups” for no other reason than spending time together, and stopping to delight in the ordinary, like crawling into bed as a family of four to watch a movie.
Normally a couple who travels frequently, we opted for things we could do with our dogs instead. We took trips to the beach, where Bill ripped through our rental property covered in sand, a road trip to Kentucky, in which both dogs decided they hated riding in the car and whined for nine hours, and visited plenty of wineries, where Bill always insisted he get the best seat in the house. What may have previously irritated me left me smiling and grateful. I look back on every photo I took during that period (more than 10,000) and I don’t see cancer; I see happiness.
Advertisement

Photo Courtesy of Kait Hanson
On a Friday morning in October 2023, Bill didn’t eat the food I put down. Instead, he looked at the bowl, looked at me, and turned around to go back to bed. I texted his oncologist: “Can you see Bill today?” On the way, Bill enjoyed his head out the window the entire time and even smiled when we pulled into spot 8. Bill loved his oncologists and care team, and whenever we got to the parking lot, no matter how he felt, it was like an internal switch was flipped and he rallied.
Throughout that day, Bill had bloodwork, ultrasounds and internal scans ― all of which came back clean showing normal lymph nodes and organs. “He looks great, all his lymph nodes palpate normally, but something is definitely off,” I remember his doctor saying as Bill rested his head on my feet. But by the end of the day, Bill was eating, wagging his tail, and ready to come home. That night, we enjoyed celebratory crab cakes and Bill, in true form, tried to steal them off our plates.
At 4 a.m. I woke up to the sound of my husband telling me something wasn’t right. Bill hadn’t slept and seemed restless. I flipped on the overhead light and one look told me this wasn’t the same dog who was attempting to eat dinner off a plate last night. We administered fluids into Bill like we’d learned to do from his care team, hoping to perk him up, but it was no use.
“Bud, just tell me what’s wrong,” I whispered into his floppy ears as dawn broke.
Our oncologist met us at the hospital, and after another thorough physical examination where Bill presented normally, we all agreed it would be in his best interest to get some supportive care in the hospital. We walked out of the hospital that morning with only his collar and leash, and it symbolized a reality I wasn’t ready or willing to accept yet.
Advertisement
“Bill won’t eat for us. I also need to let you know that his white blood cell counts and platelets are tanking,” the ICU doctor told me on the phone the next morning. “We have reason to believe his cancer has moved aggressively to his bones.”

Photo Courtesy of Kait Hanson
Puzzle pieces in my brain began shifting into place, and I suddenly felt stupid for thinking we had cheated cancer. By that night, we knew one thing for sure: Bill deserved to spend any time he had left with the people he loved most.
We brought him home and got in bed together for what would be the last time. Restless and unable to sleep, a feeling of dread nestled into my stomach. As the sun began to rise, I half hoped my lethargic best friend had done a 180 overnight, and I rubbed his back with an ounce of hope. Instead, he inched to the edge of the bed in an attempt to escape my cuddle smothering.
For more than a year, people had told us that we would know when it “was time” by the look in our dog’s eyes, a fact I had mentally filed in my brain’s “empty platitudes” folder.
Advertisement
“His eyes are a different colour,” I said to my husband when the morning light finally illuminated our room. I felt like the air was being sucked from my lungs.
That day, we pulled into the same spot that had comforted us for so long, for the last time. So much had changed since the first day we claimed spot 8 more than a year prior, and we walked into the clinic without a phone call, unmasked, and carrying the dog who once plowed through the doors. Alongside my husband and the team that had cared so deeply for him, I kissed Bill’s velvety ears as he took his last breaths.
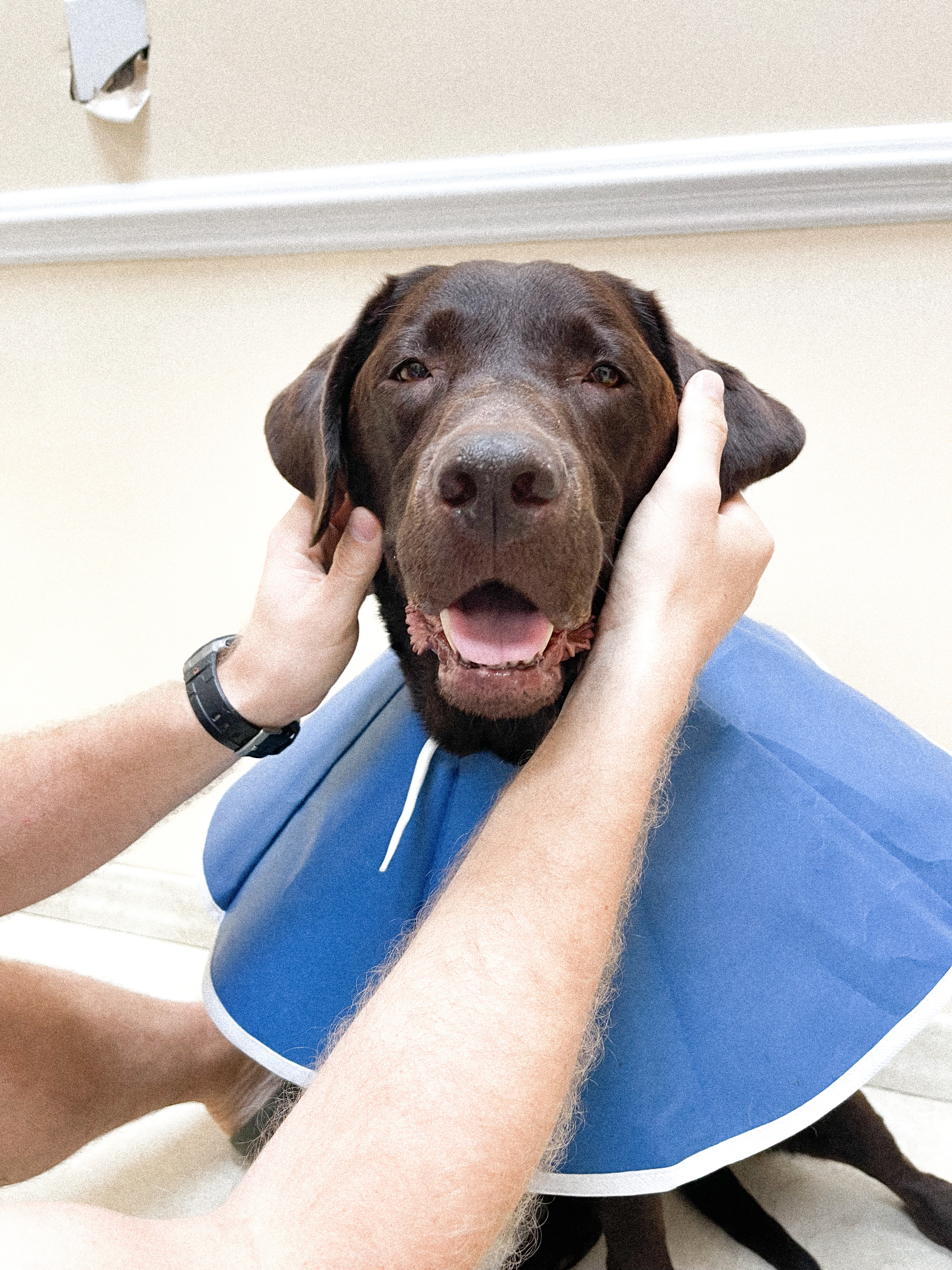
Photo Courtesy of Kait Hanson
“I feel like an idiot for being so hopeful,” I told one of Bill’s oncologists as she escorted us out of the building through a private backdoor that day.
“Hope is how you get through it,” she replied.
From the outset of his diagnosis, we had promised Bill one thing: When the bad days began to outnumber the good days, we would carry out our final act of love. At the time, we had no idea if that meant an extra month or an extra year. We stopped counting days and instead began counting moments – and we made good on our promise to him in the end without hesitation or regret. I think that was the lesson in all of this, directly from Bill himself: Life is too short not to savour every single moment and make it count.
Advertisement